Global alliances seek to develop a COVID-19 vaccine
On March 27th the UK government pledged £210 million to the Coalition for Epidemic Preparedness Innovations (CEPI) to fund the development of a coronavirus vaccine. Bill Gates, a key player in the global health sector, has donated a further $150 million to CEPI for the development of a COVID-19 vaccine. However there is a substantial shortfall in the projected funding required for the development of a viable vaccine.
CEPI is not an organisation many of us will have heard about. However it is probably one of the most important players in world health at the moment. CEPI will likely be instrumental in the development of a vaccine for the ongoing coronavirus pandemic. CEPI is a public-private partnership (PPP) between several multilateral organisations, namely the Gates Foundation and the Wellcome Trust, in addition to several government backers, including the UK. The objective of CEPI is to fund research on vaccine development for evolving diseases.
The concept of CEPI was first outlined in a 2015 paper in the New England Journal of Medicine. The paper outlined three issues surrounding vaccine development:
- The complexity of vaccine development requiring significant expertise and financial cost
- Fewer companies willing to dedicate the resources to develop and manufacture vaccines
- Problematic market incentives for manufacturers to produce vaccines for infections only with a large potential market
Diseases such as Zika and Ebola were identified as infections that have required rapid vaccine development in the past. However, given the small potential market for these vaccines these diseases have not received the necessary funding or attention from the pharmaceutical industry for the the development and manufacture of much needed vaccines. CEPI was the answer to this issue. An organisation that would provide the resources and financial stimulus to incentivise drug manufacturers to develop vaccines for emerging infections.
Fast forward two years later and CEPI was officially born at the World Economic Forum in 2017. That year, Bill Gates, the largest funder for CEPI said that he hoped the organisation would be able to significantly reduce the time to develop a vaccine by 90%, from 10 years to 1 year.
CEPI has had several tasks to deal with since its inception in 2017 but none as big as the ongoing coronavirus pandemic. Earlier this month, CEPI called for $2 billion of new funding for the development of a novel coronavirus vaccine. Bill Gates and a number of countries, including the UK’s pledge of over £200 million, answered the call. As of 19th March 2020, CEPI has began funding with eight partners to develop a COVID-19 vaccine. To date, CEPI has provided a total of $29.2 million thus far. In initial funding to Curevac, Inc., Inovio Pharmaceuticals, Inc., Moderna, Inc., Novavax, Inc., The University of Hong Kong, The University of Oxford, The University of Queensland and Institut Pasteur to develop a vaccine.

However a viable vaccine for COVID-19 is some way off as many vaccines are still in the pre-clinical phase and are yet to begin trials in humans. It is hoped that a marketable vaccine will be available within 12-18 months. Whilst this is shy of Bill Gate’s 12 month CEPI objective for vaccine development, it is a far accelerated version compared to a potential 10 year wait for a vaccine. CEPI has highlighted that it is able to rapidly incentivise public-private partnerships to increase our responsiveness to global pandemics by providing the financial resources to drive technical innovation in the pharmaceutical sector.
The United States seeks to go it alone
The United States (US) has chosen not to invest in CEPI and has forged its own path in funding research on coronavirus vaccines. The US recently signed a $456 million award to Johnson & Johnson, a large US based pharmaceutical company, for the development of a vaccine. The research, still in the pre-clinical stage, is part of a $1 billion co-ordinated partnership between the US government and the pharmaceutical sector. However, this partnership comes after less co-operative actions in the vaccine market by the US government.
Two weeks ago, the US government offered $1 billion to buy a German company, one of the frontrunners in the race to develop a COVID-19 vaccine. The offer came with the clause that any vaccine would be “only for the US”. The move was confirmed by the German foreign minister and health minister who both looked unfavourably on the US government’s unilateral grab for a potential vaccine. The company CureVac, which is currently funded by CEPI, declined the offer. The company’s largest investor commented:
“We want to develop a vaccine for the whole world and not individual countries.” (Dietmar Hopp, CureVac’s largest investor in March 2020)
In other news, the US Secretary for Health and Human Services and former pharmaceutical company executive, Alex Azar said that he would not guarantee an affordable vaccine for COVID-19. Economically this move makes sense; price limits would reduce the financial incentive for drug manufacturers to produce a vaccine and consequently reduce the intensity and speed of vaccine research. However this would reduce access to the vaccine for those without health insurance, or those unable to pay out-of-pocket for the vaccine.
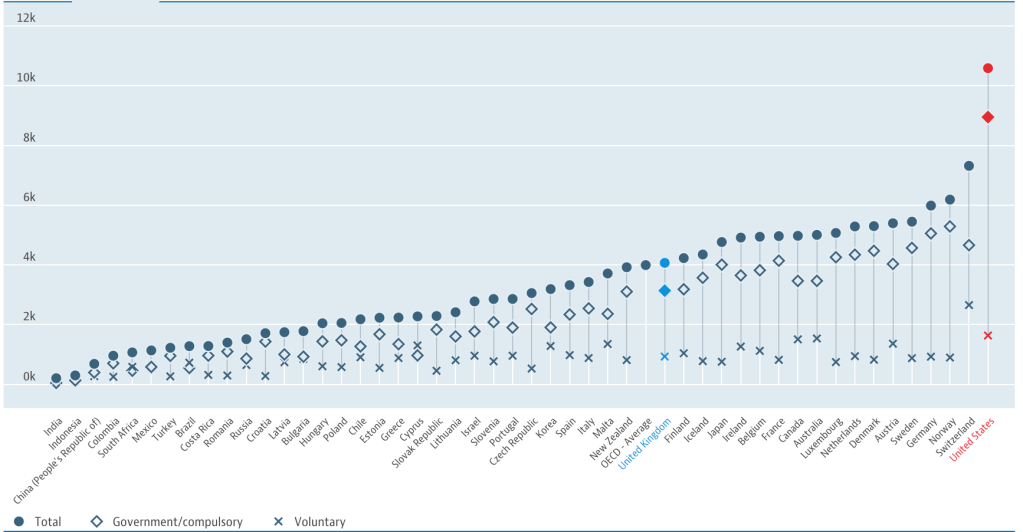
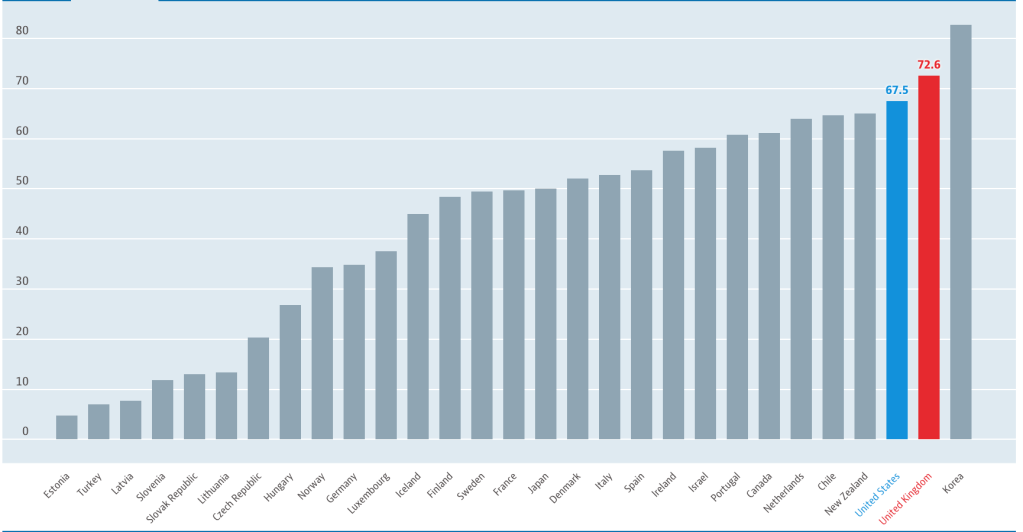
The US spending on healthcare per person far exceeds any other country in the world. Despite spending 2.5 times as much for healthcare per person than the UK, the US has poorer health outcomes. Life expectancy in the US (78.6 years) falls short of the UK (81.3 years) by 2.7 years with higher rates of obesity and metabolic diseases in the US. Despite this US citizens have fewer doctors’ consultations per person each year, a proxy for healthcare access. More worryingly poor healthcare access in the US has translated to lower vaccination rates for at risk groups in the US than the UK.
The case for higher drug pricing is clear for driving increased market incentives to create a coronavirus vaccine. However, a more expensive vaccine is likely to lead to 27.5 million US citizens living without health insurance (8.5% of the total population) being priced out from being vaccinated against COVID-19 during this global pandemic. Lower vaccination rates and reduced access to a coronavirus vaccine is likely to become an increasing issue during a time when unemployment is rising rapidly and many are facing the prospect of losing their health insurance. This is likely to have detrimental socioeconomic consequences for the US, as more people are unemployed or die due to coronavirus.
Conclusion
Time will only tell whether co-operation and partnership or unilateralism and market forces will prevail in the creation of a vaccine for the COVID-19. Whichever it is, I hope that the much needed vaccine will be delivered in a timely and equitable manner. Being a scientist at heart I have high hopes that the scientific community can come together to design, develop and manufacture a readily available vaccine. I just hope that vaccine is available and accessible to all who need it.
More One Doc’s Stories:
- How to get tested for COVID: Our household’s story
- Using military tactics to fight the war against COVID-19: How we are using age old military tactics to fight the feud against coronavirus
- Protecting healthcare workers during a pandemic: How are need to do more to protect those at the frontlines
- Dealing with a pandemic on a budget: How the world’s largest refugee camp is set up to deal with the outbreak


7 thoughts on “Developing a vaccine for COVID-19: A tale of two approaches”